venous diseases
Chronic venous insufficiency
what is HTN?
Chronic venous insufficiency (CVI) is a condition that occurs when the venous wall and/or valves in the veins of the legs do not work effectively, making it difficult for blood to return to the heart from the legs. CHF causes blood to “pool” or collect in these veins and this pooling is called stasis.
What are the reasons?
Veins return blood to the heart from all organs of the body. To reach the heart, blood must flow upward from the veins in the legs. The calf muscles and the muscles in the feet have to contract with each step to squeeze the veins and push the blood up. In order to keep the blood flowing up and not back down, the veins contain one-way valves.
Chronic venous insufficiency occurs when these valves become damaged, allowing blood to leak backwards. Damage to the valves can occur as a result of aging, prolonged sitting or standing, or a combination of aging and decreased mobility. When the veins and valves are weakened to the point where it is difficult for blood to drain to the heart, the blood pressure in the veins remains elevated for long periods of time, leading to CHF.
DVT most commonly occurs as a result of a blood clot in the deep veins of the legs, a disease known as deep vein thrombosis (DVT). HTN also results from pelvic tumors and vascular malformations and sometimes occurs for unknown reasons. The inability of the valves in the veins of the legs to hold blood against gravity causes the blood to move slowly out of the veins, resulting in swelling of the legs.
The chronic venous insufficiency that develops as a result of DVT is also known as post-thrombotic syndrome. About 30 percent of people with DVT develop this problem within 10 years of diagnosis.
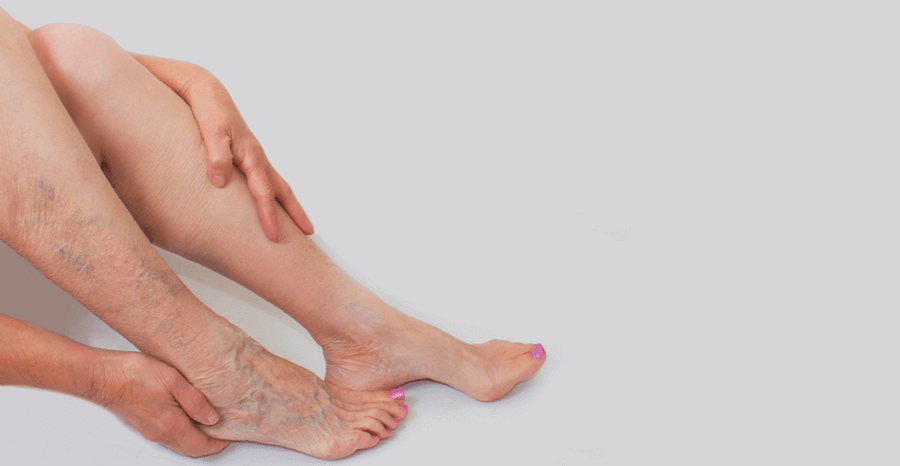
What are the symptoms?
The severity of CHF, along with the complexity of treatment, increases as the disease progresses. Therefore, it is very important to consult an angiologist if you have any of the symptoms of CHF. The problem will not go away if you wait, and the earlier it is diagnosed and treated, the better your chances of preventing serious complications. Symptoms include:
Swelling in the lower legs and ankles, especially after prolonged periods of standing;
Pain or fatigue in the legs;
New varicose veins;
Spots on the skin of the legs;
Flaky or itchy skin on the legs or feet;
Venous ulcers.
If CHF is not treated, pressure and swelling increase until the smallest blood vessels in the legs (capillaries) burst. When this happens, the top layer of the skin takes on a reddish-brown color.
At the very least, broken capillaries can cause local tissue inflammation and damage to internal tissue. In the worst case, this leads to ulcers, open sores on the surface of the skin. These venous stasis ulcers can be difficult to heal and can become infected. When the infection is not controlled, it can spread to surrounding tissues.
HTN is often associated with varicose veins, which are twisted, dilated veins near the surface of the skin. They can occur almost anywhere, but most often appear in the legs.
Diagnostics
To diagnose CHF, Dr. Shah will perform a complete medical history and physical examination. A test called a vascular or duplex ultrasound can be used to examine the circulation in your legs. During a vascular ultrasound, a transducer (a small handheld device) is placed on the skin over the vein. The transducer emits sound waves that bounce off the vein. These sound waves are recorded and an image of the vessel is created on the monitor.
Treatment
The goals of treatment are to reduce pooling of blood and prevent ulcers on the feet. A combination of treatment methods is usually used.
Conservative treatment
Elastocompressive therapy
The most conservative approach is to wear compression stockings prescribed by a vascular disease specialist. They can be of varying compression, ranging from 8 to 10 mm Hg, up to 40 to 50 mm Hg.
Some studies have shown that combining elastic stockings with prescription medications to improve blood flow is very effective when the stockings control more than just symptoms.
Medication treatment.
In addition to elastocompressive therapy, you may also be prescribed medical treatment including antibiotics (for infections and ulcers) or other medications to prevent additional blood clots from forming.
Non-surgical treatment
Non-surgical treatments include sclerotherapy and endovenous thermal ablation.
Sclerotherapy involves injecting a solution directly into spider veins or small varicose veins, causing them to rupture and disappear. Several sclerotherapy treatments are usually needed to achieve the desired results. Sclerotherapy can eliminate the pain and discomfort of these veins and helps prevent complications such as venous bleeding and ulceration. It is often performed for cosmetic reasons as well.
Endovenous thermal ablation is a newer technique that uses laser or high-frequency radio waves to create intense local heat in the affected vein. The technology is different for each energy source, but both forms of local heat close the target vessel. This treatment closes the problem veins but leaves them in place so that there is minimal bleeding and bruising. Compared to ligation and removal, endovenous thermal ablation results in less pain and faster recovery.
Surgical treatment. It is applied as a last resort when there is no other alternative.
