Venous diseases
venous wounds
What are venous wounds?
Venous ulcers, also called stagnation, insufficiency or varicose ulcers, are the result of malfunctioning of venous valves, which leads to an increase in pressure in the veins. They usually appear along the leg. The resulting venous hypertension causes blood to collect when it is not as efficiently pumped back to the heart, otherwise known as venous insufficiency. The increase in pressure stretches the walls of the veins, which allows proteins in the blood and blood cells to radiate into the subcutaneous tissues, which leads to edema and eventual disintegration of said tissues due to lack of oxygen and nutrients. Specifically, deposits around the capillaries of protein fibrin, which normally plays a role in clotting, prevent oxygen and nutrients from entering the surrounding muscles and tissues and, in turn, lead to necrosis and ulcer.
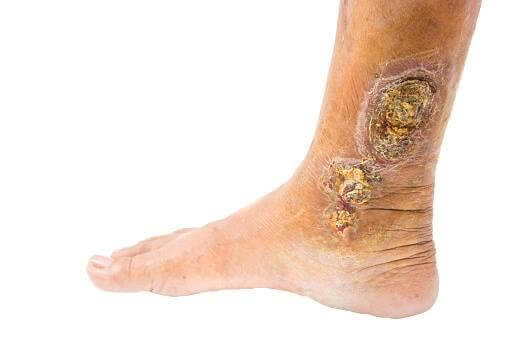
What are the symptoms?
With a venous ulcer, itching or redness is often felt, and the leg around it can be swollen. Other signs may include:
Rash or dry skin;
Brown discoloration of the skin;
Secretion with an unpleasant odor from the wound;
The ulcer can also become infected.
If this happens, you may notice:
- Redness or swelling of the surrounding skin
- Increasing pain
- Fever
- Pusta
What are the reasons?
Any condition that causes blood to pool in the leg veins is a potential cause of venous ulcers, including varicose veins, deep vein thrombosis, or heart failure. Most venous ulcers are caused by venous valves that do not properly prevent the return flow of blood or venous reflux from the deep veins back to the superficial veins located between the skin and muscles. In addition, any condition leading to muscle weakness in the lower leg in turn can reduce the effectiveness of skeletal muscle in moving blood back to the heart.
Risk factors
- Diabetes mellitus;
- Congestive heart failure;
- Peripheral vascular disease;
- Deep vein thrombosis;
- Pregnancy;
- over-fullness.
Complications
One of the most typical complications associated with ulcers of venous insufficiency is an infection of the affected tissue.
diagnostics
- Ankle-Brachial Index (ABI) to determine if there is also arterial insufficiency;
- Doppler ultrasonography;
- Venography.
Treatment
In the direct treatment of venous ulcers, the main goals are to preserve the site of the ulcer without infection during the healing process and relieve swelling. Usually, oral antibiotics are needed only if there is an infection in the surrounding tissue. The environment of the wounds should usually be moist, with bandages changing as rarely as possible due to the fact that changing the bandages removes both healthy cells and debris. In extreme cases, surgical skin grafts may be used to allow anomalously large or painful venous ulcers to heal properly.
In addition to treating the superficial wound and edema, the secondary goal in the treatment of venous ulcers is to relieve the underlying condition. One of the most common treatments is compressive therapy, which serves to reduce the diameter and pressure of blood vessels, increase efficiency, and in turn prevent venous reflux. However, compression should only be used in patients without significant arterial disease.
… and a few tips
There are different ways you can prevent venous ulcers through lifestyle changes, diet, or medications. The measures that will help you are:
- Quit smoking;
- Control your weight;
- Control chronic conditions such as high blood pressure or diabetes.
- Take aspirin to prevent blood clots.
- Reduce the amount of salt in your food.
- Exercise regularly;
- Wear compressive socks;
- Keep your feet elevated when you can.
