venous diseases
deep vein thrombosis
what is a DVT?
Deep vein thrombosis (DVT) occurs when a blood clot (thrombus) forms in one or more of the deep veins in your body, usually in your legs. Deep vein thrombosis can cause leg pain or swelling, but can also occur without symptoms .
Deep vein thrombosis can develop if you have certain medical conditions that affect how your blood clots. This can also happen if you are not moving for a long time, for example after an operation or accident or when you are bedridden.
Deep vein thrombosis can be very serious as blood clots in your veins can break off, pass through your bloodstream and reach your lungs, blocking blood flow (pulmonary embolism).
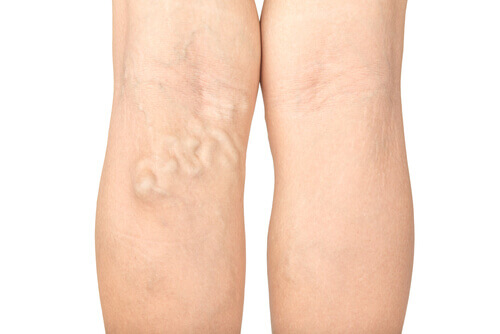
What are the symptoms?
Signs and symptoms of deep vein thrombosis may include:
Swelling in the affected leg. Rarely there is swelling of both legs.
Pain in the leg. Pain often starts in the calf and may feel like cramps or soreness.
Red or discolored skin on the foot.
Sensation of warmth in the affected leg.
Deep vein thrombosis can occur without noticeable symptoms.
What are the reasons?
The blood clots of deep vein thrombosis can be caused by anything that prevents your blood from circulating or clotting normally, such as an injury to a vein, surgery, certain medications, and restricted movement.
How to protect ourselves?
Measures to prevent deep vein thrombosis include:
– Avoid sitting still. If you have had surgery or have been bedridden for other reasons, try to get moving as soon as possible. If you sit for a while, do not cross your legs, which can interfere with blood flow. If you travel a long distance by car, stop every hour and walk around.
•If you are on a plane, stand or walk occasionally. If you can’t do that, exercise your legs. Try raising and lowering your heels while keeping your toes on the floor, then lift your toes with your heels are on the floor.
Make lifestyle changes. Control your weight and quit smoking.
•Exercises. Regular exercise reduces the risk of blood clots, which is especially important for people who sit a lot or travel frequently.
Risk factors
Many factors can increase the risk of developing deep vein thrombosis (DVT). The more you have, the greater the risk of DVT. Risk factors include:
- Hereditary bleeding disorder. Some people inherit a disorder that makes their blood clot more easily. This condition alone cannot cause blood clots unless combined with one or more risk factors.
- Prolonged immobilisation, for example during a long stay in hospital or paralysis. When your legs remain stationary for a long time, the calf muscles do not contract to help blood circulation, which can increase the risk of blood clots.
- Injury or surgery. Injury to your veins or surgery can increase your risk of blood clots.
- Pregnancy. Pregnancy increases the pressure in the veins in the pelvis and legs. Women with an inherited clotting disorder are particularly at risk. The risk of blood clots from pregnancy can last up to six седмици след като сте родили бебето си.
- Birth control pills (oral contraceptives) or hormone replacement therapy. Both can increase your blood’s ability to clot.
- Overweight or obese. Being overweight increases the pressure in the veins in your pelvis and legs.
- Smoking. Smoking affects blood clotting and circulation, which can increase the risk of DVT.
- Cancer. Some forms of cancer increase substances in your blood that cause your blood to clot. Some forms of cancer treatment also increase the risk of blood clots.
- Heart failure. This increases the risk of DVT and pulmonary embolism. Because people with heart failure have limited heart and lung function, the symptoms caused by even a small pulmonary embolism are more noticeable.
- Inflammatory bowel disease. Bowel diseases, such as Crohn’s disease or ulcerative colitis, increase the risk of DVT.
- Personal or family history of deep vein thrombosis or pulmonary embolism. If you or someone in your family has had one or both of these, you may be at greater risk of developing DVT.
- Age. If you are older than 60, you increase your risk of DVT, although it can occur at any age.
- Sitting for long periods of time, for example when driving or flying. When your legs remain still for hours, the calf muscles do not contract, which normally helps blood circulation. Blood clots can form in the calves of the feet if the calf muscles are not moved for long periods.
Complications
Pulmonary embolism
A pulmonary embolism occurs when a blood vessel in your lung becomes blocked by a blood clot (thrombus) that reaches your lung from another part of your body, usually your leg.
Pulmonary embolism can be life-threatening. It is important to watch yourself for signs and symptoms of pulmonary embolism and seek medical attention if they occur. Signs and symptoms of pulmonary embolism include:
- Sudden shortness of breath
- Chest pain or discomfort that gets worse when you take a deep breath or cough
- Feeling dizzy or fainting
- Fast pulse
- Cough up blood
Postphlebitic syndrome
A common complication that can occur after deep vein thrombosis is known as postphlebitic syndrome, also called postthrombotic syndrome. Damage to your veins from a blood clot reduces blood flow to the affected areas, which can cause:
- Constant swelling of the feet (edema)
- Pain in the leg
- Skin discoloration
- Skin inflammations
Diagnostics
To diagnose deep vein thrombosis, you will be given a physical examination to check for swelling, heaviness or change in the colour of your skin. Depending on the likelihood that you have a blood clot, your doctor may suggest tests including:
Blockade. A wand-like device (transducer) placed over the part of your body where there is a clot sends sound waves into the area. As the sound waves travel through your tissue and bounce back, the computer converts the waves into a moving image on a video screen. A clot can be seen in the image.
Sometimes a series of ultrasound examinations are performed over several days to monitor the condition of the thrombus.
Blood test. Almost all people who develop severe deep vein thrombosis have an elevated blood level of a substance called D-dimer.
Venography. Contrast is injected into a large vein in your foot or ankle. The X-ray creates an image of the veins in your legs to clots are detected. However, less invasive diagnostic methods, such as ultrasound, can usually confirm the diagnosis.
CT or MRI scan. Or it can provide visual images of your veins and can show if you have a clot. Sometimes these scans, done for other reasons, reveal a clot.
Treatment
The treatment of deep vein thrombosis (DVT) is aimed at preventing the clot from enlarging and preventing it from breaking off and causing a pulmonary embolismand subsequently reducing your chances of recurrent deep vein thrombosis.
Treatment options for deep vein thrombosis include:
Blood thinners. Deep vein thrombosis is most often treated with anticoagulants, also called blood thinners. These drugs, which can be injected or taken as pills, reduce your blood’s ability to clot. They don’t break down existing blood clots, but they can prevent clots from increasing and reduce the risk of more clots developing.
Cloisters. If you have a more serious type of deep vein thrombosis or pulmonary embolism, or if other medicines don’t work, your doctor may prescribe medicines that break down clots quickly, called thrombolytics.
Filters. If you can’t take blood thinners, you can have a filter placed in a large vein – the vena cava – in your abdomen. A vena cava filter prevents clots from forming and depositing in your lungs.
Compressiоn socks. To prevent swelling associated with deep vein thrombosis,elasto-compressive therapy is applied, by wearing socks of different compression.
This reduces the chances of your blood pooling and clotting.
