venous diseases
varicose veins
what are varicose veins?
Varicose veins are twisted, dilated veins. Any superficial vein can become enlarged, but the most commonly affected veins are those in your legs. This is because walking and standing upright increases the pressure in the veins of the lower body.
For many people, varicose veins and spider veins – a common, mild variation of varicose veins – are simply a cosmetic problem. For other people, varicose veins can cause pain and discomfort. Sometimes varicose veins lead to more serious problems.
Spider veins are similar to varicose veins, but they are smaller. Spider veins are located closer to the surface of the skin and are often red or blue. They usually appear on the legs, but can also be found on the face. They vary in size and often resemble spider webs.
When to see a doctor?
Self-care – such as exercise, elevating the legs or wearing compression stockings – can help ease the pain of varicose veins and may prevent them from getting worse. But if you’re concerned about how your veins look and feel, and the measures you’ve taken aren’t giving you the result you’re looking for, see your doctor.
What are
the symptoms?
Varicose veins may not cause pain. Signs that you may have varicose veins include:
Veins that are dark purple or blue in color
Veins that look twisted and bulging
When painful signs and symptoms occur, they may include:
Burning, throbbing, muscle cramps and swelling in the lower legs
Pain after prolonged sitting or standing
Itching around one or more of your veins
Discoloration of the skin around a varicose vein
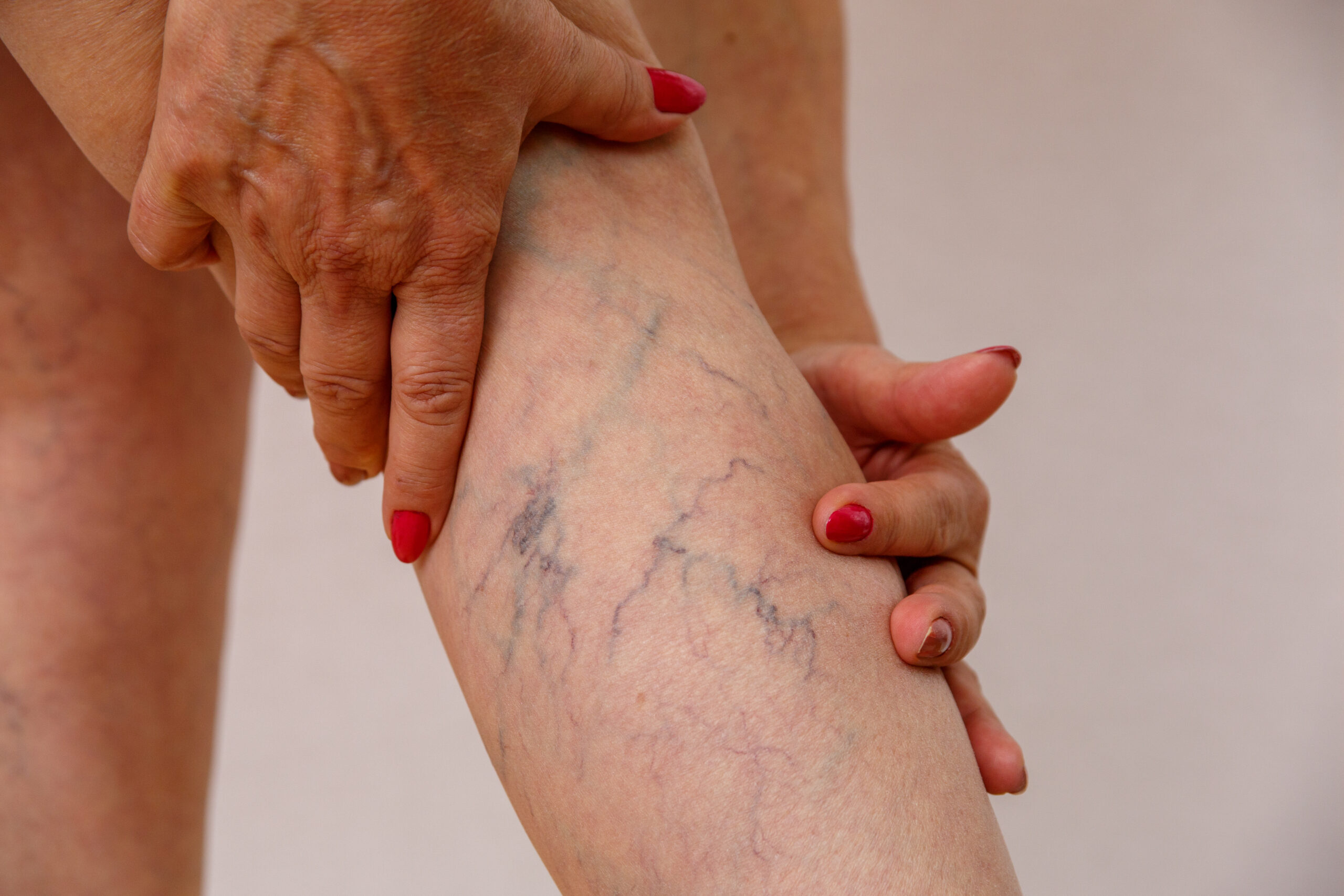
What are the reasons?
Weak or damaged valves can lead to varicose veins. Arteries carry blood from your heart to the rest of your tissues, and veins return blood from the rest of your body to your heart so that blood can recirculate. To get blood back to the heart, the veins in your legs have to work against gravity.
Muscle contractions in the lower legs act as pumps, and the elastic walls of the veins help the blood return to your heart. Small valves in your veins open when blood flows to your heart, then close to stop the blood flowing backwards. If these valves are weak or damaged, blood can flow backwards and form in the vein, causing the veins to stretch or twist.
Risk factors
These factors increase the risk of developing varicose veins:
Age
The risk of varicose veins increases with age. Aging causes wear and tear on the valves in your veins that help regulate blood flow. Eventually, this wear and tear causes the valves to allow blood to flow back into your veins, where it collects instead of flowing to your heart.
Hormonal imbalance
Women are more likely to develop the condition. Hormonal changes during pregnancy, premenstruation or menopause may be a factor, as female hormones tend to relax the vein walls. Treatment with hormones, such as contraceptives, can increase the risk of varicose veins.
Pregnancy
During pregnancy, the volume of blood in your body increases. This change supports the growing fetus, but it can also lead to an unpleasant side effect – varicose veins in the legs. Hormonal changes during pregnancy can also play a role.
Family history
If other family members have had varicose veins, you are more likely to have one too.
Obesity
Being overweight puts extra pressure on your veins. Standing or sitting for long periods of time. Your blood does not flow as well if you are in the same position for long periods.
Diagnostics
Diagnosis of varicose veins is made by physical examination and ultrasound diagnosis (Doppler).
Prevention
There is no way to completely prevent the appearance of varicose veins. But improving circulation and muscle tone can reduce the risk of developing varicose veins or getting additional ones. The same measures you can take to treat the discomfort of varicose veins at home can help prevent varicose veins, including:
- Movement
- Control your weight
- Eat foods high in fibre and low in salt
- Avoid high heels and tight tights
- Lift your legs
- Change sitting or standing position regularly
Complications
Complications from varicose veins, although rare, can include:
- Ulcers Painful ulcers can form on the skin near varicose veins, especially near the ankles. The discolored spot on the skin usually starts before the ulcer forms. See your doctor right away if you suspect you have developed an ulcer.
- Blood clots. Sometimes the veins deep in the legs dilate. In such cases, the affected leg may become painful and swollen. Any persistent leg pain or swelling requires medical attention as it may indicate a blood clot, a condition known in medicine as thrombophlebitis.
- Bleeding. Sometimes veins that are very close to the skin can burst. This usually causes only minor bleeding. But any bleeding requires medical attention.
Treatment
Fortunately, treatment doesn’t usually mean a hospital stay or a long, uncomfortable recovery. Thanks to less invasive procedures, varicose veins can usually be treated on an outpatient basis.
Care for yourself
Self-care – such as exercise, losing weight, elevating the legs and avoiding long periods of standing or sitting – can relieve pain and prevent varicose veins from worsening.
Compression socks
Wearing compression socks all day is often the first approach to try before moving on to other treatments. They firmly squeeze your legs, helping the veins and muscles of your legs move blood more efficiently. The amount of compression varies by type and brand. The degree of compression can most accurately be determined by your doctor.
in pregnancy
Varicose veins that develop during pregnancy usually improve without medical treatment within three to 12 months after delivery.
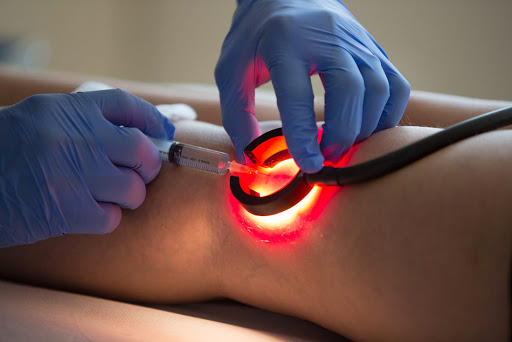
Procedures
If you do not respond to elastocompressive therapy or if your condition is more severe, your doctor may suggest one of these treatments for varicose veins:
Sclerotherapy
In this procedure, a solution or foam is injected that ruptures and closes the varicose veins. After a few weeks, the treated varicose veins should fade.Although it may be necessary to inject the same vein more than once, sclerotherapy is effective if done correctly. Sclerotherapy does not require anesthesia and can be performed on an outpatient basis.
Foam sclerotherapy of large veins
- Injecting a large vein with a foam solution is also a possible treatment for vein closure and sealing.
Catheter-assisted procedures using radiofrequency or laser energy
In these methods, a thin tube (catheter) is inserted into the enlarged vein and the tip of the catheter is heated using either radiofrequency or laser energy. As the catheter is removed, the heat destroys the vein, causing it to close. This procedure is the preferred treatment for larger varicose veins.
Ambulatory phlebectomy
Your doctor removes smaller varicose veins through a series of small punctures in the skin. In this outpatient procedure, only the parts of the leg that are pricked are listed. Scarring is usually minimal.
Endoscopic vein surgery
You may only need this surgery in a severe case involving leg ulcers if other techniques fail. A thin video camera inserted into your leg is used to visualize and close the varicose vein, and then the veins are removed through small incisions. This procedure is performed on an outpatient basis.
